Sultana Habib ( National Institute of Cardiovascular Diseases, Karachi. )
Parveen Akhter ( National Institute of Cardiovascular Diseases, Karachi. )
Salma Razzak ( National Institute of Cardiovascular Diseases, Karachi. )
Zahid Jamal ( National Institute of Cardiovascular Diseases, Karachi. )
Ishtiaq Rasool ( National Institute of Cardiovascular Diseases, Karachi. )
Khan Shah Zaman ( National Institute of Cardiovascular Diseases, Karachi. )
January 2012, Volume 62, Issue 1
Case Reports
Abstract
The case of a 60 year old male patient, diagnosed with rheumatoid arthritis presenting with recurrent massive pericardial effusion, and unresponsive to treatment of rheumatoid arthritis is documented. Pericardial biopsy proved Tuberculous pericarditis with positive fluid culture for Mycobacterium Tuberculosis. Anti-tuberculous treatment was started along with corticosteroids. Follow up after three months showed no evidence of pericardial effusion.
Keywords: Rheumatoid arthritis, Recurrent pericardial effusion, Tuberculosis.
Introduction
Tuberculosis (TB) is a common disease in Pakistan with a prevalence rate of 1% (1.5 million).1 Tuberculous pericarditis is a common and potentially lethal complication of Tuberculosis associated with a high rate of morbidity and mortality; whereas rheumatoid arthritis as pericarditis is an uncommon manifestation.2 Diagnosis of tuberculosis is usually made by isolation of acid fast bacilli (AFB) in pericardial fluid by positive AFB culture, granulomatous inflammation on pericardial biopsy, high levels of gamma INF, or raised adenosine deaminase levels.3 Treatment with antituberculous therapy and corticosteroids has a favourable prognosis. Complications include congestive cardiac failure, arrhythmias and constrictive pericarditis.
Case Report
A 60 year old male patient was admitted with complaints of fever, joint pain associated with non-radiating chest pain and increasing shortness of breath (NHYA F/C IV) with no paroxysmal nocturnal dyspnoea or orthopnoea, for the previous two weeks. He had a history of polyarthritis involving both small and large joints with morning stiffness since the last 10 years. There was no past history of chest disease.
On clinical examination, he was febrile with pulsus paradox, had distended neck veins and a raised JVP. There was no peripheral oedema, hepatomegally or lymph adenopathy. There was decreased intensity of all heart sounds with no added sounds or murmurs. He had swan neck deformity of the thumb and ulnar deviation of hands.
Bony deformaties of the patient due to rheumatoid arthritis:
Laboratory results showed increased ESR at 83 mm. ECG (Echocardiogram) showed low voltage complexes. X-ray revealed cardiomegaly with no evidence of pulmonary TB.
Echocardiogram showed a moderate to large pericardial effusion with right ventricular (RV) collapse. Pericardiocentesis was done and approximately 400 ml of turbid fluid was removed which had glucose of < 5mg%, protein of 6900mg%, leukocyte count of 2500/mm3 with 80% Polymer Pronuclear Leukocytes (Polys) and 20% lymphocytes. Gram stain and bacterial culture were negative. Cytology displayed acute and chronic inflammatory cells.Prelimanary report for acid fast bacilli (AFB) culture was negative.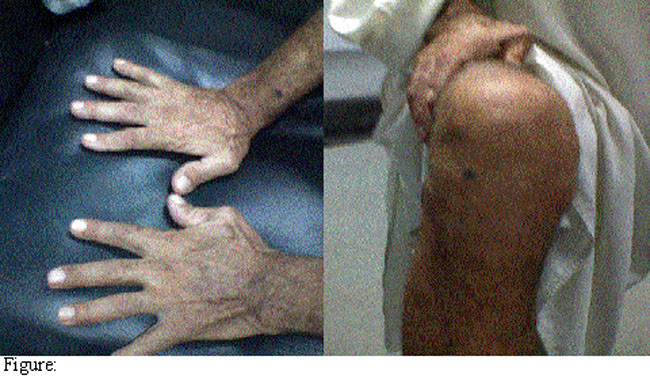
Since the patient was not taking any medication for RA, pericardial effusion appeared to be secondary to RA. This was favoured by pericardial fluid DR (direct report) and negative bacterial culture. Methotrexate (MTX) and Prednisolone was started after rheumatologic consultation, and re-accumulation of fluid in pericardium twice with development of cardiac temponade after 2 months of therapy. Pericardiocentesis fluid showed same composition and gram stain and culture report were awaited. For definite diagnosis, pericardial biopsy was done, which showed chronic granulomatous inflammation with granulomas composed of epitheloid cells, multinucleated giant cells and areas of necrosis. Meanwhile pericardial fluid AFB C/S report was also received which was found to be positive for growth of mycobacterim tuberculous sensitive to all first line anti-tuberculous therapy (ATT).
Patient was started with four ATT (rifampicin, INH, pyrazinamide, and ethambutol) and steroids, and was followed up after 6 and 12 weeks. Repeat echocardiogram showed only minimal pericardial effusion with no evidence of constriction.
Discussion
Tuberculosis is a major health problem through out the world and accounts for two million deaths each year. About 8 million new cases of tuberculosis appear each year,4 and 95% of the cases of active T.B come from Africa, Asia and Latin America which homes 86% of total world\\\'s population.1 Pakistan ranks 6th in terms of estimated number of cases by WHO with an incidence of 175/100,000. In a population of 144 million people 1.5 million are affected with T.B, indicating a prevalence rate of about 1% while 260,000 new cases appear each year.1
Although tuberclous pericarditis is a rare complication, it is increasingly found in immunosuppressed patients. Extra pulmonary T.B. occurs in 20% of patients of tuberculosis, and tuberculous pericarditis is seen in 1-8% of these patients which rises to over 50% in people on immmuno suppression therapy.3 It remains a serious condition as there is a high incidence of progression to constrictive pericarditis with a high mortality rate.5
TB pericarditis has varying clinical presentations; usually with fever, night sweats, fatigue, weight loss, chest pain and breathlessness.Pericarditis can present without any previous history of exposure to TB. In some cases chronic cardiac compression results in heart failure. Cardiac tamponade may present as a complication of pericardial effusion.6 In our case the patient had atypical symptoms with the absence of fever, night sweats or weight loss. Moreover, pericardial fluid had predominant polys on cytology, and low glucose which is why it was initially treated as a pericardial effusion secondary to rheumatoid arthritis.
Definitive diagnosis of tuberculous pericarditis is usually made by one or more of the following criteria:6
*Isolation of mycobacterium tuberculosis in pericardial fluid or biopsy.
*Demonstration of granulomatous inflammation on histopathological examination of pericardial biopsy sample.
*PCR (gold standard diagnostic test) in cases where other tests are negative.
*Isolation of mycobacterium tuberculosis from sputum or non pericardial effusion exudates in the presence of radiological and/or clinical evidence of tuberculosis associated with a positive response to anti-tuberculous therapy and in the absence of any other obvious causes of pericarditis.
Medical literature search did not reveal any similar cases. Keeping in view the high incidence of TB in Pakistan diagnosis was confirmed on the basis of a pericardial biopsy and positive AFB culture.Antituberculous therapy comprising of four drugs Isoniazid, Rifampicin, Pyrazinamide and Ethambutol for at least 2 months was given, followed by Isoniazid and Rifampicin for another 4 months which proved highly effective. Treatment for 9 months or longer usually gives no better results.7 The effectiveness of corticosteroids in T.B pericarditis remains controversial. Three clinical trials with a total of 326 participants were assessed for effectiveness of adjunctive steroids in tuberculous pericarditis.8 A study by Strang et al showed that corticosteroids group experienced more rapid clinical improvement, a lower rate of requirement of pericardectomy (in case of constrictive pericarditis) and a lower mortality rate from pericarditis at 24 months versus placebo group; but these findings were not statistically significant.9 Early diagnosis, anti-TB chemotherapy,and high doses of steroids has shown to decrease the incidence of pericardial constriction and mortality following TB pericarditis.10
Conclusion
Tuberculous pericarditis can present with recurrent PE without any history or symptoms of TB.A high index of suspicion should be maintained in every case of PE in our population. Repeated samples for analysis and isolation for mycobacterium tuberculosis may be more productive than a single sample. When available PCR should be the choice of investigation. PCR testing may decrease the number of cases classified as idiopathic.
References
1.WHO. Country Profile. Pakistan; Global Tuberculosis Control 2003; pp 99-101.
2.Lebowitz WB. The heart in rheumatoid arthritis (Rheumatoid disease). A clinical and pathological study of sixty-two cases.Ann Intern Med 1963; 58: 102-23.
3.Zayas R, Angnita M, Torres F, Gimenez D, Bergillos F, Ruiz M, et al. Incidence of specific etiology and role of methods for specific etiologic diagnosis of primary acute pericarditis. Am J Cardiol 1995; 75: 378-82.
4.Murray JF.A century of tuberculosis. Am J Respir Crit Care Med 2004; 169: 1181-6.
5.Desani HN.Tuberculous pericarditis: a review of 100 cases. S Afr Med J 1979; 55: 877-80.
6.Mayosi BM, Burgess LJ, Doubell AF. Tuberculous pericarditis: Heart diseases in Africa. Circulation 2005; 112: 3608-16.
7.Combs DL, O\\\'Brien RJ, Geiter LJ. USPHS Tuberculosis Short-course therapy Trial21: effectiveness, toxicityand acceptability: the report of final results. Ann Intern Med 1990; 397-406.
8.Akim JG, Ternouth I, Mushangi E, Siziya S,Robertson V, Malen A. A Double blind randomized placebo controlled trial of adjunctive prednisolone in treatment of effusive pericarditis in HIV sero positive patients. Heart 2000; 84: 183-4.
9.Fanning A. Tuberculosis:Exra pulmonary disease. CMAJ 1999; 160: 1597-603.
10.American Thoracic Society: CDC; Infectious Diseases Society of America. Treatment of Tuberculosis.MMwr Recomm Rep 2003; 52 (RR-11): 1-77.
Journal of the Pakistan Medical Association has agreed to receive and publish manuscripts in accordance with the principles of the following committees:




